What is Vein Disease?
Find relevant information here.
Current Page →
What Is Lymphedema of the Legs?
The lymphatic system is a network of vessels, nodes, and ducts that collect and circulate excess fluid in the body. Fluids pass from capillaries to be absorbed by lymphatic channels and lymph nodes, which act as filters to stop infections. Lymphedema is swelling in a body part caused by inefficient fluid drainage by the lymphatic system, resulting in buildup of lymphatic fluids most commonly in the arms or legs. Lymphedema happens when the lymphatic system is damaged or ineffective and cannot remove fluid. People develop lymphedema for many reasons, including genetic abnormalities (primary lymphedema or vascular malformation), surgery and lymph node removal, radiation and chemotherapy, infections, obesity, trauma, heart/liver/kidney problems, and chronic venous disease (phlebolymphedema).
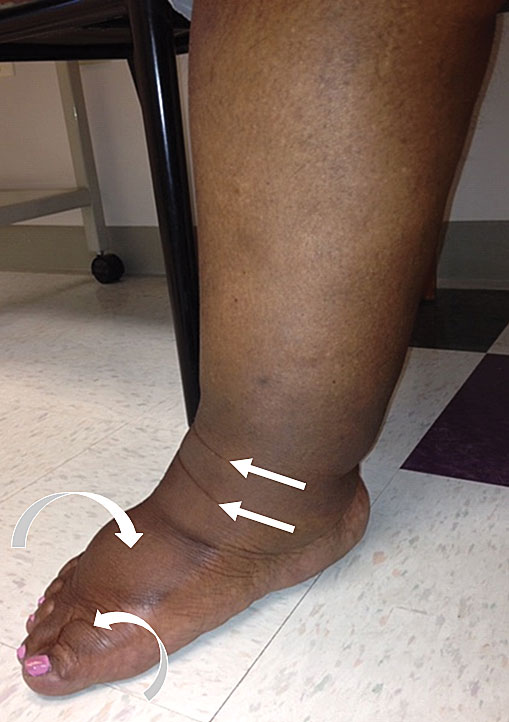
Lymphedema of the leg and foot. Swelling of the leg can cause skin creases (straight arrows) which makes wearing compression stockings difficult because the stocking material can fold into the creases. Swelling of the foot and toes (curved arrows) is not seen in venous edema (The Healthy Veins Book, 2023, p. 192, fig. 37-2).
What Are the Symptoms and Signs of Leg Lymphedema?
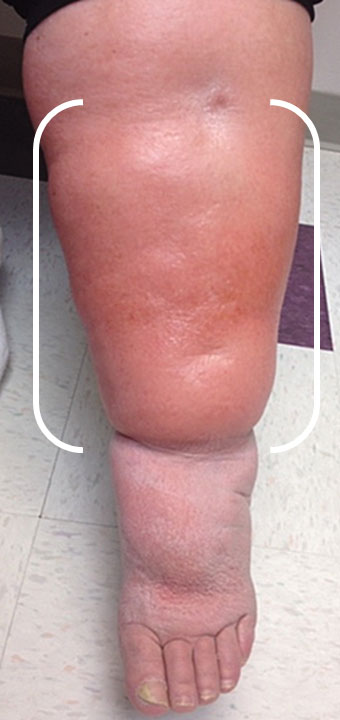
Symptoms of leg lymphedema include swelling of one or both legs, always involving the foot and toes, as well as heaviness and fatigue. These symptoms may be present upon awakening and worsen as the day progresses. Initially, determining if mild swelling is lymphedema (Grade 1) may be difficult, as it responds to leg elevation and compression stockings. Skin cracks, blisters, and weeping make it susceptible to infections as the condition progresses (Grade 2). In the most advanced cases (Grade 3/4), compression cannot reduce swelling and the skin becomes hard and irregular (fibrotic) and discolored.
How is Lymphedema Diagnosed?
First, your physician or non-physician provider will ask you about your symptoms and about your medical history. They will also do a physical exam and may order blood work. An ultrasound of the veins may be ordered to assess for venous disease as a possible cause. A heart ultrasound or echocardiogram may be ordered if you have heart failure symptoms. To assess the blood vessels or deeper structures in your abdomen and pelvis, your provider might order a CT scan or MRI. Finally, a lymphoscintigram may be ordered, where dye is injected into the foot to allow the lymphatic system to be seen.
How is Lymphedema Treated?
Lymphedema is often a chronic disease that needs lifelong attention. The first thing a physician or non-physician provider does when you are diagnosed with lymphedema is manage the symptoms of edema and skin problems and initiate a workup for potential treatable causes. Compression stockings are a mainstay of therapy and can help. For more advanced cases, short stretch bandages such as Velcro wraps or multilayer bandaging are needed. An additional modality to treat lymphedema is massage therapy or manual lymphatic drainage (MLD), which is done by a certified lymphedema therapist (CLT) and continued at home by the patient.
Another at-home treatment is pneumatic compression with a lymphatic pump. The legs are inserted into sleeves that inflate sequentially and provide gentle active compression of the lymphatic system. Skin needs to be moisturized, clean, and protected from cuts, abrasions, and sunburns. Exercise, leg elevation, and avoiding long periods of inactivity are also important.
Surgery is rarely done for lymphedema, although select advanced cases can be treated with liposuction or microsurgery of lymphatic vessels and channels by surgeons who specialize in these procedures. Successful treatment for lymphedema depends on the patient’s acceptance of and compliance with the prescribed treatments.
Chapter 37: Lymphedema of the Legs