January/February Issue of Vein Specialist
SCAI, SIR, and SVS Jointly Publish Proceedings from Multispecialty Peripheral IVUS Roundtable

Patrick Muck, MD
Chair, AVF Continuing Education Committee
AVF Representative to the IVUS Roundtable
Proceedings from an expert consensus roundtable that discussed the benefits of intravascular ultrasound (IVUS) in lower extremity revascularization procedures were released in the Journal of the Society for Cardiovascular Angiography & Interventions (JSCAI), Journal of Vascular and Interventional Radiology (JVIR), and Journal of Vascular Surgery – Vascular Insights.
The roundtable focused on the current challenges in diagnosing and treating lower extremity revascularization, knowledge and data gaps, and the potential role of IVUS in addressing these challenges. Experts shared their insights and experiences from the fields of interventional cardiology, interventional radiology, and vascular surgery. The expert consensus meeting was convened by SCAI and co-sponsored by: American Vein and Lymphatic Society (AVLS), American Venous Forum (AVF), Society of Interventional Radiology (SIR), Society for Vascular Medicine (SVM), and Society for Vascular Surgery (SVS).
“Improvements in outcomes following peripheral vascular intervention have lagged compared to other endovascular treatments, such as percutaneous coronary intervention. Both clinical experience and evidence support the greater use of peripheral IVUS to reduce adverse events and extend the patency of our lower extremity revascularization procedures. By gathering experts from different specialties, we aimed to foster collaboration and exchange ideas to improve patient care for peripheral IVUS,” said Eric A. Secemsky, MD, MSc, FSCAI, lead author of the proceedings document and Director of Vascular Intervention, Beth Israel Deaconess Medical Center. “The roundtable provided a unique opportunity to identify knowledge gaps and discuss how IVUS can enhance our understanding and treatment of peripheral arterial and deep venous pathology.”
Lower extremity revascularization is a critical procedure used to restore blood flow to the legs and feet in patients suffering from peripheral arterial disease (PAD) and deep venous pathology. It is estimated that millions of people worldwide are affected by these conditions, which can lead to severe pain, non-healing wounds, and even limb loss if left untreated. Although angiography is the dominant imaging modality in revascularization, it has inherent limitations. IVUS is a minimally invasive imaging technique that allows physicians to visualize the inside of blood vessels in real-time. It provides detailed information about the vessel wall, plaque composition, and blood flow characteristics, enabling more accurate diagnosis and treatment planning.
During the roundtable, participants highlighted the potential of IVUS in guiding revascularization procedures, such as angioplasty and stenting, to optimize outcomes for patients. They also emphasized the need for further research and evidence to support the integration of IVUS into routine clinical practice.
“This multidisciplinary roundtable collaborated to highlight the importance of IVUS in venous interventions and to help shape future clinical guidelines. IVUS clearly improves the ability to treat patients afflicted with venous disease leading to better outcomes and quality of life,” said Patrick E. Muck MD RVT FACS, Chief of Vascular Surgery, Program Director Vascular Fellowship & Integrated Residency, Co-Director Venous Thromboembolic Therapies at Good Samaritan Hospital in Cincinnati, OH.
The roundtable concluded with a commitment to ongoing interdisciplinary collaboration and knowledge sharing among physicians. Participants agreed that treatment standards, formal training programs and global quality metrics remain needed to improve patient care.
The considerations and consensus views shared in “Intravascular Ultrasound Use in Peripheral Arterial and Deep Venous Interventions: Multidisciplinary Expert Opinion From SCAI/AVF/AVLS/SIR/SVM/SVS” represent the opinion of the consensus committee members.
Sources:
Secemsky EA, Aronow HE, Kwolek CJ, et al. Intravascular ultrasound use in peripheral arterial and deep venous interventions: multidisciplinary expert opinion from SCAI/AVF/AVLS/SIR/ SVM/SVS. J Soc Cardiovasc Angiogr Interv. Published online January 9, 2024. doi: 10.1016/j.jscai.2023.101205.
https://doi.org/10.1016/j.jscai.2023.101205
Secemsky, EA, Aronow HD, Kwolek, CJ, et al. Intravascular ultrasound use in peripheral arterial and deep venous interventions: multidisciplinary expert opinion from SCAI/AVF/AVLS/SIR/SVM/SVS. J Vasc Interv Radiol 2024. https://www.jvir.org/; published online January 9, 2024. doi: 10.1016/j.jvir.2023.11.006
https://doi.org/10.1016/j.jvir.2023.11.006
Secemsky, EA, Aronow HD, Kwolek, CJ, et al. Intravascular ultrasound use in peripheral arterial and deep venous interventions: multidisciplinary expert opinion from SCAI/AVF/AVLS/SIR/SVM/SVS. JVS-Vascular Insights. Published online January 9, 2024. doi: 10.1016/j.jvsvi.2023.100033.
Sumner Session to Launch Leadership Development Program

John Forbes, MBA
Executive Director, American Venous Forum (AVF)
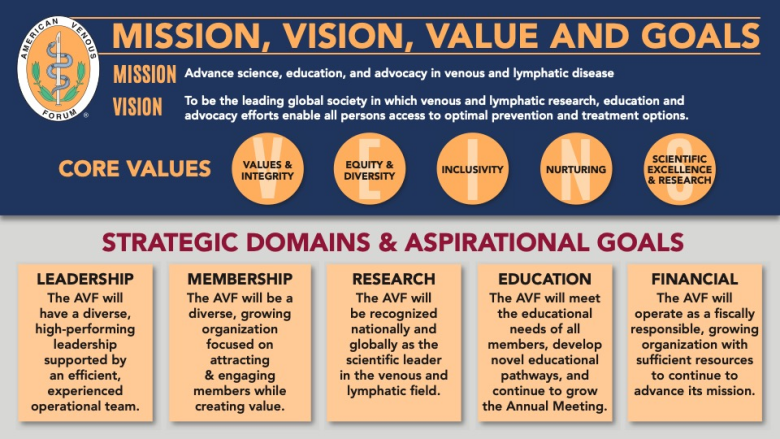
In June 2023, American Venous Forum President, Glenn Jacobowitz, MD convened a strategic planning retreat of the AVF’s Board of Directors. With inputs from many AVF stakeholders including past presidents, committee leaders, members, and industry representatives the Board spent a day and a half envisioning the future of the AVF, developing aspirational goals, prioritizing objectives and identifying potential initiatives that would comprise our strategic plan. The graphic below incorporates our mission, vision, core values and aspirational goals and is the highest-level representation of the new strategic plan.
Bill Marston, MD
Chair, AVF Strategic Planning Committee
Immediate Past President, AVF
“The new strategic plan is a living, breathing roadmap of the future of the AVF.”
A key element of the new strategic plan is leadership. The AVF Board understands that for the AVF to be successful we must invest in our current and future leaders. Ruth Bush, MD, President-elect of the AVF, along with a group of outstanding AVF leaders will be introducing some of the critical components of leadership during the Sumner Session at VENOUS2024 in Tampa, Florida. The session is scheduled on Monday, March 4th beginning at 3:30pm ET.
| Sumner Session
Leadership Mastery: Navigating Challenges and Inspiring Growth Moderated by Ruth Bush, MD |
|
|---|---|
Faculty:
|
Topics to be covered:
|
Don’t miss the Sumner Session and hear from top AVF leaders about their leadership journeys.
In addition to the Sumner Session, the AVF Board has selected two junior members of the Board of Directors to participate in a nearly year-long leadership development program hosted by the Society of Vascular Surgery (SVS). Misaki Kiguchi, MD and Mikel Sadek, MD will be joining the sixth cohort of individuals who have participated in SVS’ leadership development program.

Misaki Kiguchi, MD
Member, AVF Board of Directors

Mikel Sadek, MD
Member, AVF Board of Directors
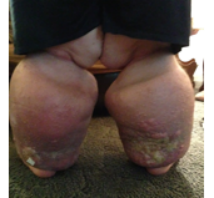
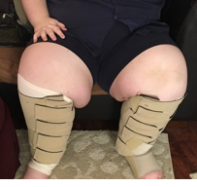
Medicare Coverage Expanded to Include Lymphedema Compression Supplies in 2024

Carmen Anderson
Reimbursement & Market Access Consultant for USMCA
The United States Medical Compression Alliance (USMCA), composed of Essity, Juzo, Lohmann & Rauscher, medi, and Sigvaris – is a collaborative effort to improve the standard of care for the venous and lymphatic patient populations by providing medically prescribed gradient compression garments and supplies. The organization took large strides in 2023 to support implementation of the Lymphedema Treatment Act, a pivotal piece of legislation passed by Congress in December 2022 that created a new Medicare benefit category for lymphedema compression supplies. The USMCA collaborated with lymphedema community stakeholders and focused on three crucial areas- coding, coverage, and payment- to support patient access to medically necessary products.
We worked diligently to identify appropriate codes to align with available products and patient needs.
The USMCA initially submitted HCPCS applications in June and followed up with an expanded list of HCPCS codes for CMS to consider during the rule writing period. These codes focused on textile technology (i.e., knit, adjustable wraps, nighttime, and bandages), anatomical locations throughout the body (from individual toe caps to head and neck), dosage in millimeters of mercury (mmHg), and standard or custom versions. 78 codes were published specific to lymphedema, and 3 codes were revised specific to surgical dressings.
Advocating for sufficient and fair payment rates continues to be important to the USMCA. Patient access to necessary products without financial hardship while supporting the businesses and associated services is essential. To bill Medicare for lymphedema compression garments and supplies an organization must become an enrolled Durable Medical Equipment, Orthotics, and Prosthetics (DMEPOS) supplier. The fees are structured as a single payment amount which includes the products, supplies, and all training and fitting services.
Coverage went into effect January 1, 2024 and in the absence of a medical policy, claims will be reviewed on a claim by claim basis by the Durable Medical Equipment Medicare Administrative Contractors (DME MACs). The USMCA recently hosted a virtual meeting with the DME MACs to advocate for fair and accessible coverage decisions and to share clinical perspectives from a certified lymphedema physical therapist and a vascular surgeon.
The USMCA will continue their advocacy efforts and navigate the changing landscape through education and strategic initiatives to support all stakeholders in the journey toward improved lymphedema care and access to products and services. Please visit our website for additional resources and future updates.