Vein Specialist
2026The Great Masquerader
When Things Aren’t What They Seem

The Great Masquerader: When Things Aren’t What They Seem
Imaging is central to the management of many patients, from diagnosis through treatment. We have become reliant on imaging to “give us the answer.” Most of the time, it gives us the correct answer and is indispensable in our ability to care for large numbers of patients with increasing clinical complexity. However, we are reminded every so often that imaging, and really any test, is just that–a test. It cannot take the place of the greatest device in all of medicine, the human mind. We must approach all problems with an open mind, exercise curiosity, and be persistent to ensure that we are doing best for our patients. What follows is a case where things just weren’t what they seem.
The patient is female, in her early 30’s, with a history of childhood retinoblastoma and lymphoma. She has been cancer-free for decades. She presents with rapid onset of right lower extremity edema. No pain is associated with the edema, and the swelling worsens throughout the day. There is no prior history of deep vein thrombosis.
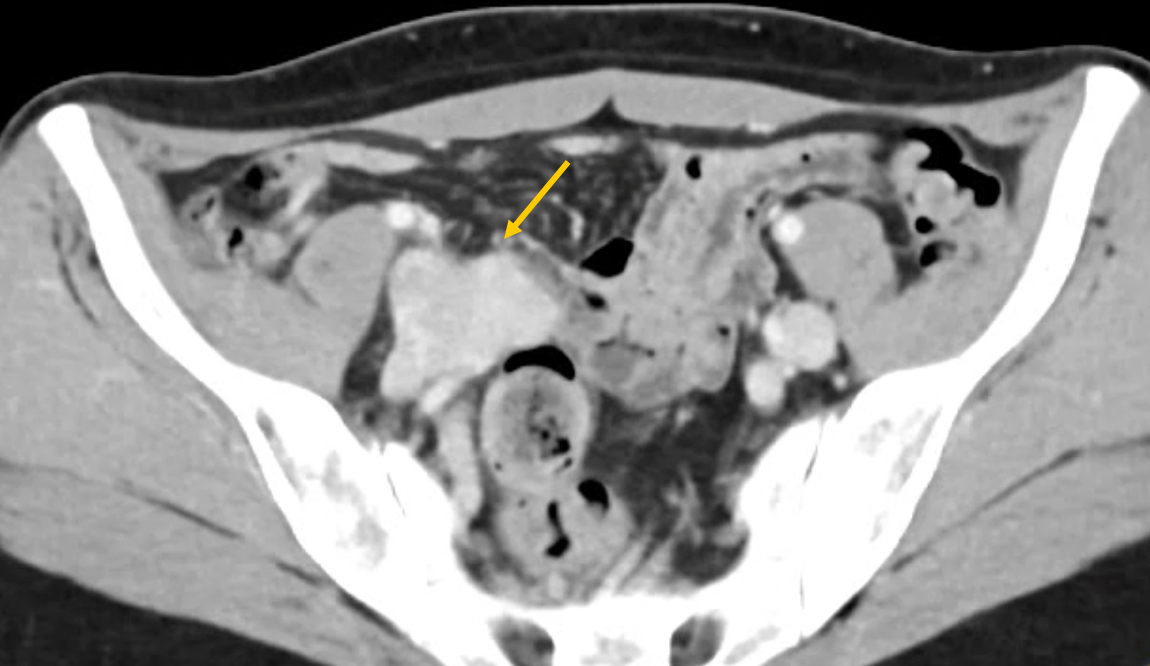
A lower extremity venous duplex ultrasound is performed and is negative. A computed tomographic venogram is obtained and demonstrates a lobulated lesion in the right iliac fossa; the differential diagnosis given was venous aneurysm, vascular malformation, and possibly a mass (Figure 1, yellow arrow). Her primary care physician initiates enoxaparin and sends her to us for consultation.
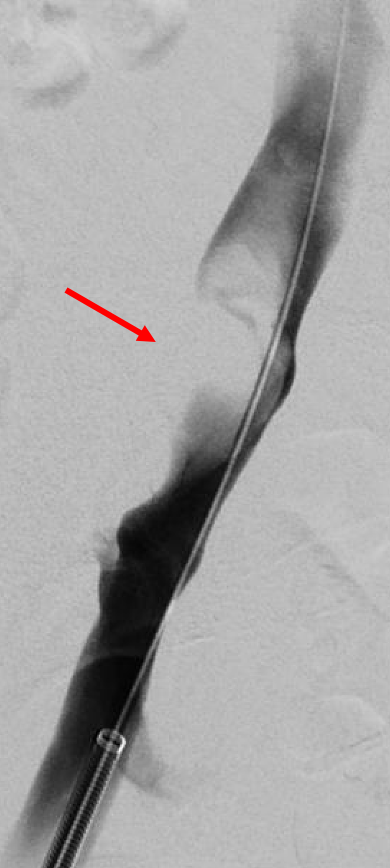
During consultation, we discuss that we should proceed with venography to characterize the nature of this lesion. Venography is performed, demonstrating a filling defect in the right external iliac vein (Figure 2, red arrow). However, it does not have the appearance of thrombus, as it appears eccentric, almost wall-attached.
An attempt is made with a guide catheter to perform suction; if this is bland thrombus, some portion should be aspirated. However, nothing could be aspirated. We then consider the final possibility from the initial differential diagnosis: intraluminal mass.
We consider all possibilities for biopsy, however, there was no clear, safe way to perform this from a percutaneous approach. Thus, we consider the possibility of endovascular biopsy.
The initial venogram was performed from right common femoral access and a second high right great saphenous vein access is obtained. Through the second access, an intracardiac echocardiography (ICE) catheter is introduced and used to image the mass as shown in Figure 3; the mass can be visualized, along with color doppler identification of the adjacent right external iliac artery.
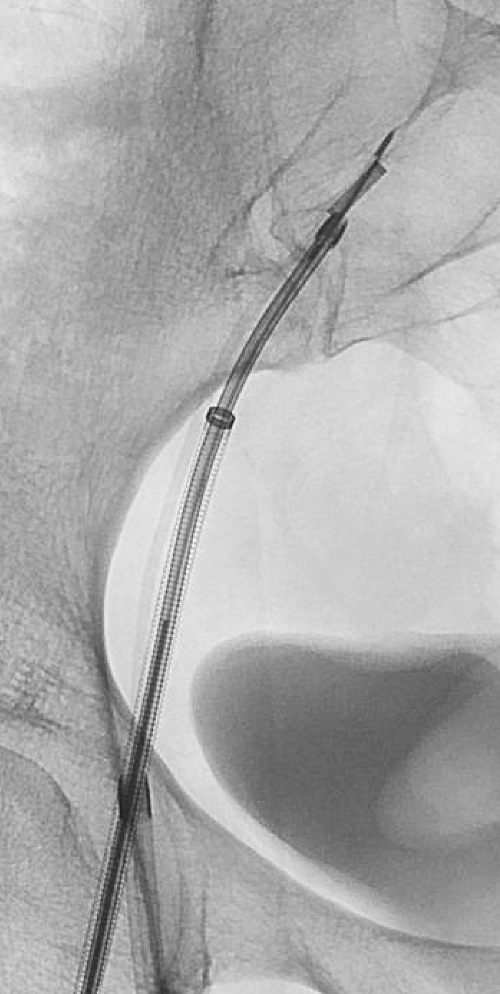
We then introduce a transjugular liver biopsy needle through the right common femoral vein access and perform endovascular biopsy using concomitant fluoroscopic and ICE guidance (Figures 4a and b). We have pathology on-site to perform adequate assessment of the specimens. The patient is diagnosed with a venous leiomyosarcoma and is referred for operative resection.
Remember to use your most important asset as a clinician – things aren’t always what they seem!
Unmasking the Masqueraders: When Leg Ulcers Aren’t What They Seem
Venous leg ulcers (VLUs) account for approximately 70% of chronic lower extremity wounds. They typically present with familiar characteristics: medial ankle (Gaiter) location, hemosiderin staining, and edema. Yet not every ulcer that looks venous is truly venous in origin. Misdiagnosis can delay appropriate treatment and lead to poor outcomes—especially when the underlying pathology is malignant, inflammatory, or metabolic. Three notable masqueraders warrant heightened clinical vigilance: dystrophic calcification, pyoderma gangrenosum, and Marjolin’s ulcer.
Dystrophic Calcification
Dystrophic calcification refers to localized calcium phosphate deposition in damaged tissues despite normal serum calcium and phosphate levels. In chronic wounds, it may present as hard, chalky deposits within the ulcer bed—often overlooked during routine lower extremity assessment. These calcifications can provoke a foreign body reaction, impair granulation, and perpetuate non-healing. While subcutaneous calcification occurs in up to 10% of patients with chronic venous insufficiency, intrawound calcification is rarer and underreported. Misdiagnosis can lead to prolonged unnecessary antibiotics and management should address concomitant venous disease with compression therapy and local wound care, but may require surgical debridement and adjunctive therapies.
Dystrophic calcinosis cutis in a patient under underlying chronic venous insufficiency s/p GSV RFA unresponsive to endovenous therapy, topical therapy, and compression. Improved once calcified tissue identified and serially sharply removed in clinic.
Pyoderma Gangrenosum
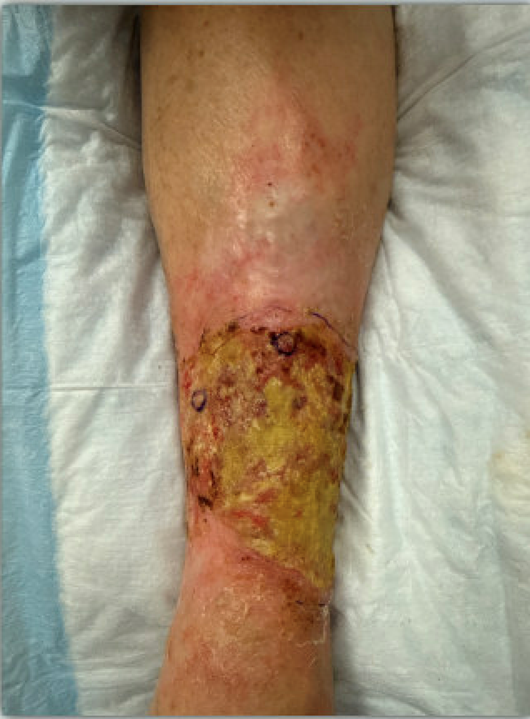
Pyoderma gangrenosum (PG) is a neutrophilic dermatosis characterized by painful, rapidly progressing ulcers with undermined violaceous borders. Though it may mimic VLUs in location and chronicity, PG typically worsens with debridement and lacks venous stasis signs; however , it is often missed in patients with VLU. Associated with systemic diseases such as inflammatory bowel disease or rheumatoid arthritis, PG requires clinical diagnosis supported by exclusion and biopsy. In PG, immunosuppressive therapy is the foundation of medical management and topical therapy must be adjusted, however simultaneous management of underlying CVD is needed.
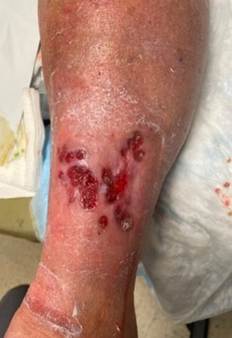
Pyoderma gangrenosum mimicking slow- to- close VLU: pathognomic features include pain out of proportion with ulcer presentation, worsening with excisional sharp debridement, and nonresponse to VLU management measures.
Marjolin’s Ulcer
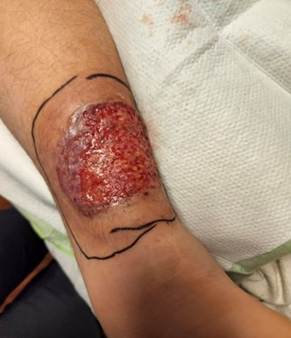
Marjolin’s ulcer represents malignant transformation—most commonly squamous cell carcinoma—within chronic wounds or scars. It may arise in longstanding VLUs, especially with repeated trauma or infection. Clinical red flags include excessive pain, raised or rolled edges, foul odor, and failure to respond to standard care. Performing a biopsy is essential. Early oncologic referral and wide excision are critical to prevent metastasis. Again, adequate management must include consideration of underlying CVD.
Marjolin’s ulcer in a patient with underling PAOD s/p tibial revascularization with concurrent GSV reflux and underlying varicosities, initially treated as PG without histologic confirmation unresponsive to all therapies. Biopsy showed squamous cell carcinoma.
Conclusion
Clinicians must maintain a high index of suspicion when evaluating chronic leg ulcers. Atypical features, poor response to standard venous therapy, or unusual wound bed findings should prompt reconsideration of the diagnosis. Performing biopsies, imaging, and seeking interdisciplinary input can differentiate true VLUs from dangerous mimics—ensuring timely, targeted care.
References
Enoch S, et al. Dystrophic calcification as a cause for non-healing leg ulcers. Int Wound J. 2005;2:142-147.
Colboc H, et al. Calcified leg ulcers in older patients. J Gerontol A Biol Sci Med Sci. 2022;77(1):27-32.
Hofmann AG, Deinsberger J, Oszwald A, Weber B. The histopathology of leg ulcers. Dermatopathology. 2024; 11(1):62-78. https://doi.org/10.3390/dermatopathology11010007
Marjolin’s Ulcer: A Rare Entity. Indian J Dermatol. 2010;55(3):301-302.
AVF 2026 in Denver: Elevating Education, Hands-On Learning, and Professional Connections
The American Venous Forum (AVF) invites clinicians, researchers, and allied health professionals of all specialties to join us February 28–March 4, 2026, in Denver, Colorado, for AVF 2026. As the premier educational event dedicated to treating venous and lymphatic disease, the annual meeting delivers high-quality, evidence-based programming designed to advance clinical practice and improve patient outcomes worldwide.
Attendees will experience a comprehensive agenda featuring expert-led plenary sessions, scientific abstract presentations, case-based discussions, and focused programming for physicians, physicians-in-training, and advanced practice providers. The meeting highlights the latest research, innovative technologies, and practical strategies that can be immediately applied in clinical settings.
A defining feature of AVF 2026 is its emphasis on hands-on learning. Interactive workshops and skills-based sessions provide participants with valuable opportunities to refine techniques, explore new devices, and gain confidence in emerging approaches to venous and lymphatic care.
Equally important are the networking opportunities woven throughout the meeting. Receptions, exhibit hall engagement, and informal gatherings create meaningful connections among peers, faculty, industry leaders, and trainees—fostering collaboration, mentorship, and professional growth.
For those unable to travel, AVF offers a virtual attendance option, ensuring access to key educational sessions and important scientific content from anywhere. This flexible format allows participants to stay engaged with the latest advances while accommodating busy schedules and travel considerations.
With its theme of “Solutions through science,” AVF 2026 promises a dynamic and inclusive experience for all specialties—bringing the global venous and lymphatic community together to learn, connect, and shape the future of patient care.
The AVF Annual Meeting:
An American Conference with an International Heart
The American Venous Forum (AVF) invites colleagues from around the world to join the premier gathering in venous and lymphatic medicine. Far from being a solely American event, the AVF annual meeting has evolved into a truly global hub, with 25% of attendees joining from outside the United States.
We have created a program that honors and integrates our international community, offering unique opportunities for education, debate, and recognition.
Our scientific agenda features dedicated sessions tailored to international perspectives:
- The International Session: This flagship session includes a keynote lecture from a world-renowned expert, presentation of complex cases for discussion, and a highly anticipated debate on the management of incompetent perforators.
- The Villavicencio Session: Named in honor of the distinguished Dr J. Leonel Villavicencio, this session highlights the best abstracts of the meeting and features interactive case discussions that promote clinical exchange.
Networking and Recognition
The AVF provides excellent opportunities to network with colleagues from every continent. We are committed to celebrating our global delegates:
- International Group Photo: Join the AVF leadership for an official group photograph commemorating the diverse community that drives our mission forward.
- Global Networking: Engage with peers from around the world to share techniques, research, and friendship.
Celebrate with Us
Beyond the science, experience our signature social events:
- Welcome Reception: Kick off the meeting by reconnecting with old friends and making new ones.
- The Celebration Apres AVF: Don’t miss this evening, a festive night dedicated to celebrating the achievements of our vibrant community. Special magic performance by Peter Glovizcki, MD.
Join us at the annual meeting of the American Venous Forum, where the world comes together to advance venous care.

Handbook of Venous and Lymphatic Disorders
Fifth Edition — Guidelines of the American Venous Forum
American Venous Forum Achieves Record Membership in 2025, Strengthening Its Global Leadership in Venous and Lymphatic Care
The American Venous Forum (AVF) closed 2025 with the highest membership in its history—an extraordinary milestone that reflects the organization’s growing influence and its unwavering commitment to advancing care for patients with venous and lymphatic disease worldwide.
This record-setting achievement represents more than a number. It signals a powerful and expanding community of physicians, advanced practice providers, researchers, and trainees dedicated to improving outcomes through education, research, advocacy, and collaboration. As venous and lymphatic disorders affect millions of patients globally, AVF’s expanding membership underscores the increasing recognition of the specialty’s importance and the need for expert-driven leadership.
Throughout 2025, AVF continued to elevate the standard of care by delivering high-impact educational programming, fostering multidisciplinary dialogue, supporting cutting-edge research initiatives, and mentoring the next generation of specialists. From scientific forums and hands-on learning opportunities to clinical guidelines and global outreach efforts, AVF remains at the forefront of innovation and evidence-based practice.
The growth in membership also reflects AVF’s inclusive and collaborative culture. By welcoming professionals across specialties and career stages—from physicians-in-training to seasoned experts—the organization strengthens its collective expertise and amplifies its global reach.
As AVF looks ahead to 2026 and beyond, this milestone reinforces its position as the leading authority in venous and lymphatic care. With a rapidly growing, engaged membership and a clear strategic vision, AVF is poised to continue shaping the future of the specialty—improving patient care, advancing science, and driving meaningful progress for the millions affected by venous and lymphatic disease worldwide.
Together, this record membership is not just a celebration of growth—it is a testament to a shared mission and a stronger future for patients everywhere.