September/October Issue of Vein Specialist
Amsel’s SCureClamp and InVera: Disruptive Medical Devices

Lowell Kabnick, MD, FACS, FAVLS, DABVLM, DFAVF
Member, AVF International Committee
SCureClamp™
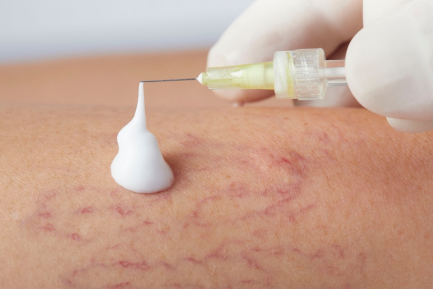
Amsel’s SCureClamp™ is a minimally invasive, needle-delivered technology which securely and permanently occludes the targeted incompetent vein in minutes with minimal patient discomfort. The technology consists of 2 nitinol clamping elements connected by a titanium rod that are delivered percutaneously through a fine (18G) needle guided by standard ultrasound imaging. The 2 occluding clamps delivered on either side of the vessel with the titanium rod transfixing the vein are like a surgically placed “transfixion suture,” preventing slippage or displacement of the clamps. The arms of the nitinol clamps interdigitate and adapt to the variable thickness and size of the targeted vein without crushing the tissues between the clamps.
Preclinical acute and chronic animal studies have confirmed the efficacy to occlude the targeted vein, and initial patient studies, with a 12-month follow-up, have confirmed the safety of implantation of the Amsel SCureClamp.
Current minimally invasive treatments, both thermal and chemical, delivered endoluminally rely on the tissue response of the vessel to occlude the vein. Long segments of venous occlusion are required, and generally take significant physician time to perform with associated patient discomfort.
The Amsel SCureClamp supplements the current approved and marketed technologies, where there is a clear unmet need in the management and treatment of chronic venous disease. This includes, but is not limited to, the treatment of perforating veins and isolated, recurrent, or “recanalized” venous segments from previous failed treatments.
InVera™ Device
Existing non-thermal methods for treating superficial venous reflux are reliant on chemical sclerosants or cyanoacrylate glue implantation. An exclusively mechanical, non-chemical, non-implant and non-thermal method presents a promising avenue for achieving a less invasive, non-tumescent treatment.
The InVera™ device* is composed of a 5Fr catheter for deployment of a nitinol helical coil that is withdrawn through the vein, exposing its outer abrasive surface to the endothelium and media layers and is subsequently recaptured and removed without catching or snagging on the vein wall. This results in venospasm, thrombosis, and subsequent fibrotic inflammatory changes similar to existing thermal and chemical ablation technologies but without their associated harmful effects.
An ovine pre-clinical study of the device in 16 representative saphenous veins (mean diameter 4.2mm, average treatment length 27cms) demonstrated impressive performance with no flow on ultrasound follow up at 6 weeks in 10 veins (63%), rising to 100% occlusion in veins treated with an optimized technique.
A European pilot clinical trial has currently enrolled 10 patients with early follow up results at 1 week demonstrating 100% occlusion and significant improvement in quality of life scores and patient reported outcomes. The exclusively mechanical treatment was well tolerated by patients with minimal pain and a strong safety profile with no significant adverse events.
As the journey from bench to bedside continues, this innovative mechanical-only ablation device holds the potential to revolutionize the treatment landscape for chronic venous disease patients.
*InVera Medical’s mechanical-only ablation catheter is still under investigation and not approved for clinical use in the US.
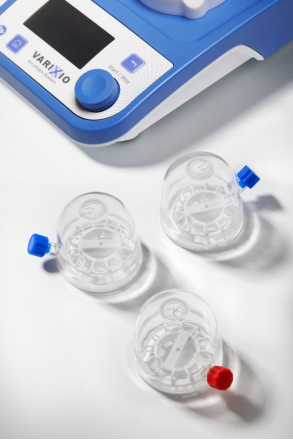
Unlocking Consistency in Sclerotherapy: The Impact of VARIXIO Technology

Adam M. Gwozdz, MD, MSc
Clinical Lecturer in Vascular Surgery, Department of Surgery and Cancer, Imperial College London
Member, AVF Research Committee
For those specializing in vein treatment, the introduction of VARIXIO® represents a meaningful step forward in the field of sclerotherapy. One of the primary challenges in sclerotherapy was the non-uniformity in foam production. Most of us are familiar with the inconsistencies stemming from manual preparation methods, often leading to variations in foam quality. These inconsistencies can influence the outcome of the procedure and the overall patient experience. VARIXIO’s automated pod system attempts to address this concern by ensuring the consistent delivery of high-caliber foam.
This becomes an exciting prospect when considering its ability to produce stable foam at low concentrations of polidocanol (POL) and sodium tetradecyl sulfate (STS). The efficacy of traditional foam in treating spider veins has been underwhelming. This limitation was attributed to the inability of existing mechanical preparation methods to generate foam at low sclerosant concentrations effectively. VARIXIO overcomes this challenge, broadening the spectrum of veins amenable to foam sclerotherapy.
I’ve been using the VARIXIO Pod system for more than a year now in an NHS setting and enjoy the workflow that it provides. The VARIXIO Pod Air system allows me to work efficiently by having multiple concentrations of sclerosant ready for me to use, depending on my application needs. The stirring programs are calibrated to optimize the foam’s quality and allow the user to define their choice of sclerosant (STS or POL), the concentration, and the type of gas used (air or a physiological mix). VARIXIO reports that the bubble diameter of the foam produced averages 100 µm and the mean half-life extends up to 5.2 min.(1) I don’t have experience with the new VARIXIO Pod Low N2, which provides a preparation system for up to 20 mL of foam made from a mix of physiological gases, which has the potential to improve the overall safety profile even further. Compared with manual foam preparation methods, cost-effectiveness has not yet been established and may be a significant consideration. However, VARIXIO’s technology provides a potent combination of quality, versatility, and safety that is worth considering for vein specialists seeking a more efficient and reliable approach to sclerotherapy.
- Roche E, Pons R, Roche O, Puig A. A new automated system for the preparation of sclerosant foam: A study of the physical characteristics produced and the device settings required. Phlebology. 2020;35(9):724-33.